- AI Software
- C3 AI Applications
- C3 AI Applications Overview
- C3 AI Anti-Money Laundering
- C3 AI Cash Management
- C3 AI Contested Logistics
- C3 AI CRM
- C3 AI Decision Advantage
- C3 AI Demand Forecasting
- C3 AI Energy Management
- C3 AI ESG
- C3 AI Health
- C3 AI Intelligence Analysis
- C3 AI Inventory Optimization
- C3 AI Process Optimization
- C3 AI Production Schedule Optimization
- C3 AI Property Appraisal
- C3 AI Readiness
- C3 AI Reliability
- C3 AI Smart Lending
- C3 AI Supply Network Risk
- C3 AI Turnaround Optimization
- C3 Generative AI Constituent Services
- C3 Law Enforcement
- C3 Agentic AI Platform
- C3 Generative AI
- Get Started with a C3 AI Pilot
- Industries
- Customers
- Events
- Resources
- Generative AI for Business
- Generative AI for Business
- C3 Generative AI: How Is It Unique?
- Reimagining the Enterprise with AI
- What To Consider When Using Generative AI
- Why Generative AI Is ‘Like the Internet Circa 1996’
- Can the Generative AI Hallucination Problem be Overcome?
- Transforming Healthcare Operations with Generative AI
- Data Avalanche to Strategic Advantage: Generative AI in Supply Chains
- Supply Chains for a Dangerous World: ‘Flexible, Resilient, Powered by AI’
- LLMs Pose Major Security Risks, Serving As ‘Attack Vectors’
- What Is Enterprise AI?
- Machine Learning
- Introduction
- What is Machine Learning?
- Tuning a Machine Learning Model
- Evaluating Model Performance
- Runtimes and Compute Requirements
- Selecting the Right AI/ML Problems
- Best Practices in Prototyping
- Best Practices in Ongoing Operations
- Building a Strong Team
- About the Author
- References
- Download eBook
- All Resources
- Publications
- Customer Viewpoints
- Blog
- Glossary
- Developer Portal
- Generative AI for Business
- News
- Company
- Contact Us
- search Search
- Generative AI for Business
- Reimagining the Enterprise with AI
- What To Consider When Using Generative AI
- Why Generative AI Is ‘Like the Internet Circa 1996’
- Can the Generative AI Hallucination Problem be Overcome?
- Transforming Healthcare Operations with Generative AI
- Data Avalanche to Strategic Advantage: Generative AI in Supply Chains
- Supply Chains for a Dangerous World: ‘Flexible, Resilient, Powered by AI’
- LLMs Pose Major Security Risks, Serving As ‘Attack Vectors’
- C3 Generative AI: Getting the Most Out of Enterprise Data
- The Key to Generative AI Adoption: ‘Trusted, Reliable, Safe Answers’
- Generative AI in Healthcare: The Opportunity for Medical Device Manufacturers
- Generative AI in Healthcare: The End of Administrative Burdens for Workers
- Generative AI for the Department of Defense: The Power of Instant Insights
- C3 AI’s Generative AI Journey
- What Makes C3 Generative AI Unique
- How C3 Generative AI Is Transforming Businesses
Transforming Healthcare Operations with Generative AI

Healthcare payers and provider groups can use generative artificial intelligence (AI) to improve the quality of care, improve the patient experience, and reduce operating costs by unlocking efficiencies in healthcare administration and operations. While healthcare services face several risks and challenges when implementing generative AI – protecting patient privacy, trusting AI answers, preventing clinical harm, and complying with healthcare regulations – those can now be overcome with generative AI designed for the enterprise, providing the level of security and transparency that healthcare organizations require. C3 Generative AI for Healthcare supports payers and provider personnel responsible for reducing gaps in care and streamlining claims management. It does so by providing consistent, accurate, and trustworthy answers to daily, time-consuming responsibilities within existing workflows. The benefits of implementing C3 Generative AI to address these opportunities include:
Implementing enterprise generative AI is easier than deploying traditional healthcare AI solutions, with fewer data complexities. The cost of not integrating generative AI into administration and operations workflows is substantial: payers, provider groups, and other healthcare organizations that fail to transform with generative AI will face a significant competitive disadvantage, both in terms of operating costs, and the quality of patient care and experience.
Addressing Potential Pitfalls
For enterprise generative AI to deliver value, it should be used by healthcare personnel in multiple roles, fulfilling different responsibilities, and with varied access to enterprise data sources. All users must trust the outputs of generative AI, and the system must explain where the answers come from; verifying and documenting decision making is a necessary component of healthcare administration and operations workflows. The following are examples where these risks arise:
Protecting Patient Privacy and Sensitive Data
A provider group COO wants to evaluate care gaps trends and revenue impact for multiple office sites. The information needed to answer these questions is stored in disparate reports and is sensitive, access restricted information. One concern is that any questions and/or answers typed into a generative AI product will be inadvertently uploaded to the internet. With C3 Generative AI, LLM processing sits behind your company’s firewall and is not connected to the internet – questions and answers will not be exposed. Another concern is if the COO can access this sensitive material, would other employees without approved access be able to see the same information? By implementing an enterprise-wide role and policy-based framework that recognizes which personnel are asking a question and what their access rights are, C3 Generative AI ensures only authorized sources are used in results.
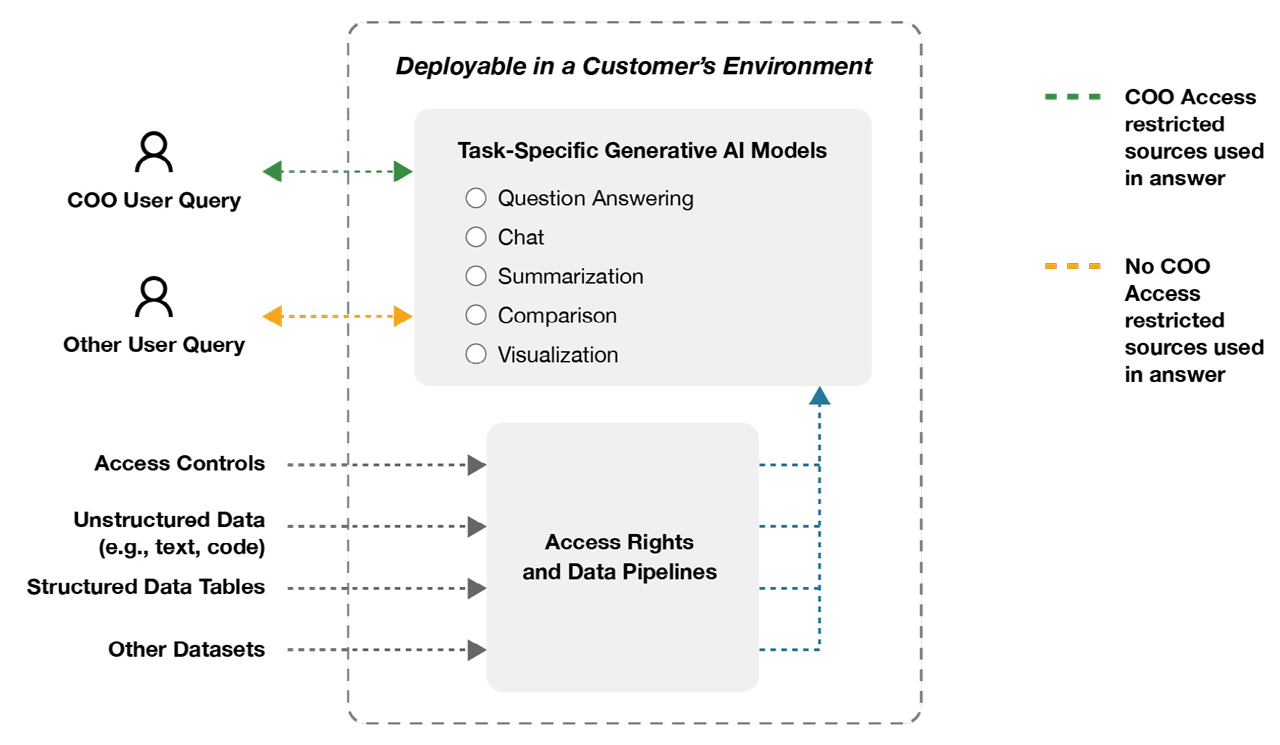
Trusting Generative AI Answers
Consider the roles of two healthcare claims managers within the same organization. Both are reviewing state regulation updates and implementing changes regarding claims and billing requirements. When each claims manager uses the generative AI product to summarize recent policy updates, responses must be consistent even when the question is phrased differently. “Hallucination” occurs when generative AI products generate false information, often because there is not any credible source data, and the LLM is programmed to produce a probabilistic answer, regardless of accuracy.
C3 Generative AI addresses these concerns by including a retrieval model that recognizes the documents and data sources that are most relevant and authorized for access. The retrieval model interacts with the LLM to summarize the information, sources included. If no applicable documents and data sources are available, the retrieval model recognizes this limitation and notifies the user – it does not provide an answer that lacks supporting data. This approach gives users the ability to review the sources provided and independently determine if the answer is appropriate and useful – avoiding black-box answers. The retrieval model also supports consistent, traceable answers by generating results from the same documents and data sources even when the question is asked slightly differently.
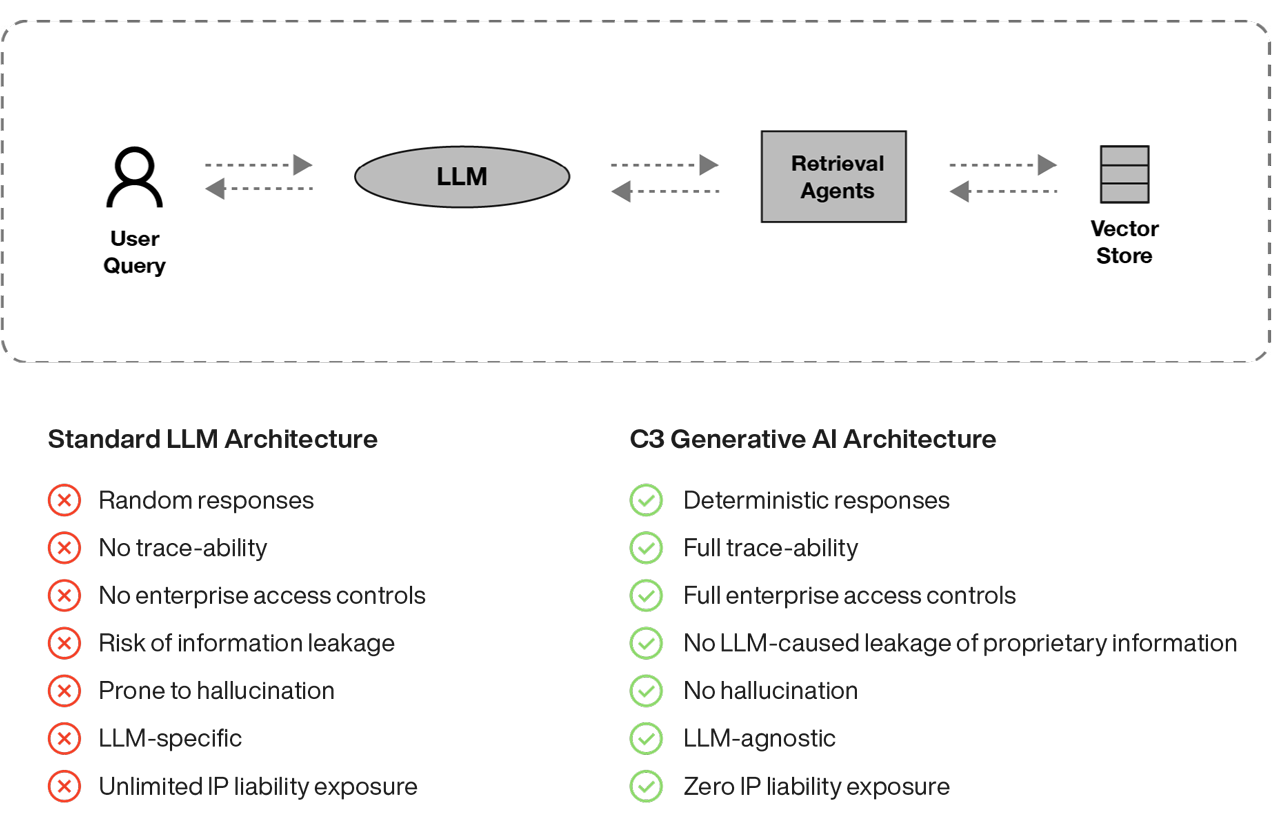
Use Cases and Implementation
Reducing Care Gaps
Gaps in care appear when the care a patient receives does not match policy or guideline recommendations, or when there is a loss in continuity of care. Recommended best practices and guidelines are frequently changing, introducing complexity in identifying and applying the latest recommendations. Analytical models, including AI, are already being used to identify preventative services and close care gaps before they happen. To efficiently close care gaps, providers and payers need to engage in bi-directional communication and documentation. Generative AI can increase productivity in this process by sourcing the latest policies and guidelines appropriate to a specific patient and automating much of the documentation and communication. The benefit of doing this is consistent, preventative, authorized care eases patient barriers to care, encourages patient engagement, and reduces healthcare costs.
Gaps in Care

A care gap coordinator can use enterprise generative AI to find care planning guidelines and educational material relevant to individual patients. This information can be shared with the patient, then summarized and documented by generative AI. The coordinator will also contact providers to inform them of patient care gaps and any related upcoming appointments. Generative AI can assist in summarizing and documenting communication to and from providers to help reduce time spent completing these essential tasks. Accurate and fast communication to patients and providers regarding care gaps will lead to a better patient experience and improved quality of care.
Streamlining Claims Management
Claims management is an intensive, and time-consuming daily task to document care, and to determine cost responsibilities between the patient and healthcare provider. It is a multi-step process to document what care was provided and why. That information is then reviewed and distilled into the key events and codes necessary to process a claim. A claims processor then conducts further review to ensure exactly what should be covered by health insurance for each policy holder. This end-to-end process is laborious and error-prone, leading to poor patient experience and high operating costs. Generative AI can increase productivity by summarizing and highlighting clinical notes, lab results, and other medical documents.
A medical coder can use enterprise generative AI to accurately summarize services, documenting the medical data sources in the process, and transforming the services into medical codes to share with insurance plans. This will reduce the time and effort required to complete medical coding, while also reducing errors in an increasingly complex medical coding system. Providing medical coders with generative AI will improve the overall patient experience by reducing the claims management wait time.
Summary
Applying C3 Generative AI for Healthcare to payer and provider operations will establish a competitive advantage by empowering personnel and improving the patient experience. Trusting generative AI answers and protecting sensitive information are core requirements to supporting multiple healthcare roles and responsibilities that are realized by sourcing results and implementing enterprise-wide access controls. Implementing generative AI today is critical to prepare for enterprise-wide transformation tomorrow.



